|
6/17/2023 0 Comments Left olecranon fracture Nondisplaced olecranon fractures can be treated with an initial period of immobilization in a posterior slab long arm splint with the elbow in 45-90 degrees of flexion followed by early progressive active range of motion exercises with avoidance of active extension. The reduction is indicated in type 3 injuries with the aim of reducing the remaining articular surface with the trochlea. After a thorough history, physical exam, and imaging, the fracture should be immobilized in a posterior splint with slight extension. Suspected olecranon fractures require orthopedic consultation. Type I injuries account for 5-12% of cases and approximately 6% are type III injuries. The most common fracture pattern is Type II, which occurs in 80-85% of olecranon fractures. This injury is a fracture-dislocation, collateral ligaments may be incompetent causing instability. In type III injuries the fracture is displaced and the ulno-humeral joint is unstable. Type II fractures are displaced at least 3mm, however, the ulno-humeral articulation is maintained indicating intact collateral ligaments. The goal of this system was to simplify the classification of olecranon fractures based on fracture comminution, displacement, and stability of the ulno-humeral joint. There are three types, each one further subdivided into type A and B, indicating non-comminuted and comminuted respectively. The most commonly used is the Mayo classification first described by Morrey in 1993. There are several classification systems of olecranon fractures. Computed tomography (CT) may be used in complex fracture patterns with associated injuries for pre-operative planning. Images should be examined for associated coronoid, radial head fracture or dislocation, and ulno-humeral congruity. 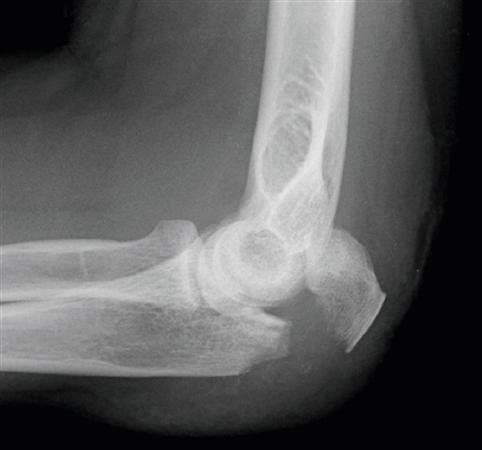
A dedicated radiocapitellar view may also be performed to evaluate for radial head and capitellum fractures. Initial evaluation with anteroposterior (AP) and lateral radiographs of the elbow are sufficient for most fractures to determine fracture pattern. It is prudent to question the patient about other sources of pain and examine all four extremities for crepitus, deformity, or pain with range of motion. When the injury occurred secondary to a high-energy mechanism, the practitioner should be vigilant to avoid missing injuries that may be unrecognized by the patient due to the distracting nature of the olecranon fracture. The examiner should palpate the elbow as well as the adjacent joints. A complete upper extremity neurovascular examination of the involved extremity should be conducted. The ulnar nerve is most at risk due to its superficial position on the medial aspect of the elbow. It is important to examine the entire involved extremity for associated injuries or lacerations suggestive of an open fracture.Īssociated injuries of the coronoid process, radial head, or proximal radioulnar joint (Monteggia fracture) may be present and evaluated for on radiographs. The examiner must ensure that the patient is not using gravity to mimic active elbow extension. This is typically done by abducting the shoulder to 90 degrees, supporting the upper arm, and asking the patient to straighten their elbow from this position. The hallmark of an olecranon fracture is the inability to extend the elbow against gravity. If the fracture is displaced there may be marked deformity at the elbow with a palpable gap. Patients typically present with elbow pain and swelling following a fall. Awareness of these structures is key when operating in this region. The ulnar nerve lies on the medial aspect, posterior to the medial collateral ligament before crossing anteriorly to run alongside the ulnar artery. Unstable injuries require reduction and stable fixation of the olecranon to restore elbow stability. Olecranon fractures can have associated with ligamentous injury (the medial and lateral collateral ligaments stabilize against valgus and varus stress respectively), coronoid process, and radial head fractures. The olecranon confers stability to the elbow joint, acting as a block to the anterior translation of the ulna in relation to the distal humerus. Greater displacement suggests tearing of the fibrous sheath over the olecranon. The pull from the triceps is the key deforming force, pulling the separated fragment superiorly. A displaced fracture interrupts the extensor mechanism resulting in loss of active elbow extension. The triceps muscle (innervated by the radial n) inserts onto the olecranon, blending with the periosteum. In fractures with significant comminution, inadvertent malreduction by narrowing the greater sigmoid notch may further predispose the patient to arthritis. Posttraumatic arthritis occurs in approximately 20% of cases and persistent malreduction >2mm of the articular surface is associated with this outcome. 
Olecranon fractures typically involve the articular surface of the elbow. 
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
